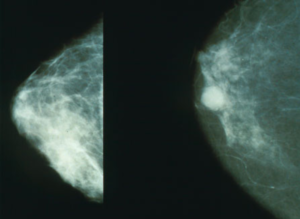
Reports of the death of Cost-Effectiveness Analysis in the U.S. may have been exaggerated: The ongoing case of Mammography
Guidelines for the use of mammograms to screen for breast cancer have been the topic of one of the fiercest and longest-running debates in medicine.







