
Don’t pave the cow paths: The challenge of re-conceptualizing health care processes
There is a popular adage for information technology professionals: “Don’t pave the cow paths.” I recently worked with a client from Texas, and they were

There is a popular adage for information technology professionals: “Don’t pave the cow paths.” I recently worked with a client from Texas, and they were

Trinity Health – Michigan and Blue Cross Blue Shield of Michigan (BCBSM) recently announced that they signed a three and a half year agreement under which
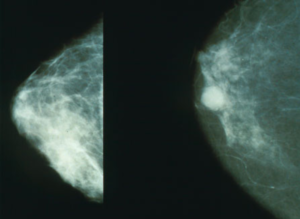
Guidelines for the use of mammograms to screen for breast cancer have been the topic of one of the fiercest and longest-running debates in medicine.
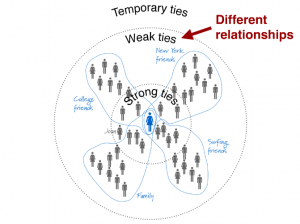
Few things in my work life are better than finding mind-blowing information from other industries and figuring out the implications for healthcare. I recently read

Ron Klar, MD, MPH is a health care consultant with a long history of involvement in federal health care policy and health plan innovation. He
Presentation entitled “Developing the Economic Model for Success” from day 2 of the American Medical Group Association’s Accountable Care Organization Learning Collaborative, at the Swissotel

Ron Klar, MD, MPH is a health care consultant with a long history of involvement in federal health care policy and health plan innovation. He
According to an article in Healthcare IT News, an advisory panel that is shaping measures for the next stage of meaningful use has suggested delaying

Today I attended a webcast sponsored by the Bipartisan Policy Center, an organization “committed to the art of principled compromise.” The webcast featured Farzad Mostashari, MD,

I went to the huge HIMSS’11 convention in Las Vegas a few weeks ago. When visiting the bewildering number of vendor booths, I focused on