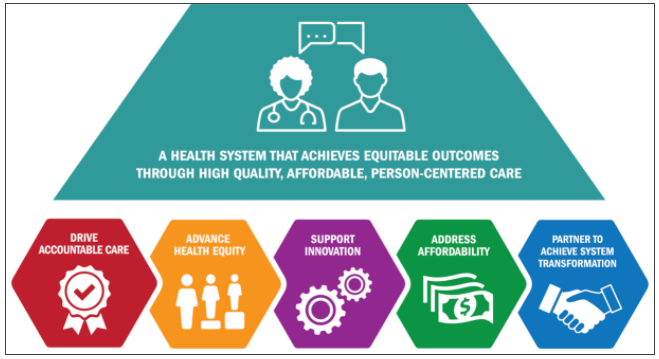
There are five methodological domains that support the measurement component of the care process improvement process:
- Population needs assessment involves the characterization of various patient populations, including demographics, risk factor profile, disease incidence and prevalence, and health care utilization patterns to identify opportunities for improvement and to support data-driven prioritization of clinical practice improvement efforts.
- Effectiveness research involves the measurement of physiologic impact, health outcomes and cost of alternative strategies for diagnosis and treatment of a particular condition to inform clinical decision-making and to support the process of clinical policy-making. Effectiveness research can sometimes be accomplished through observational studies, but frequently requires randomized clinical trials to overcome sources of bias that threaten the inferences drawn from observational studies.
- Program evaluation involves establishing the performance characteristics and effectiveness of strategies for clinical practice improvement or organization of care to support decisions about the future role of these strategies. Program evaluation allows for the comparison of what did happen after implementing the program with what would have happened had the program not been implemented. In summary, population needs assessment is a tool to support priority setting, while effectiveness research and program evaluation are tools to support decision-making about how to achieve improvements.
- Clinical practice profiling, also known as internal performance reporting, involves the characterization of clinical performance, in terms of quality of care, utilization and patient satisfaction. Such profiles can be case mix adjusted, and are often used to support internal accountability of clinicians and clinical leadership. Feedback of cost or utilization data to clinicians has been shown to lead, in certain situations, to reduction in cost and utilization of diagnostic tests.
- External performance reporting involves the characterization of clinical performance, in terms of quality, utilization, satisfaction, and health outcomes to support external accountability to employers, insurers and other constituencies. As with clinical practice profiles, external performance reports can be case mix adjusted.
For almost all of these domains, a spectrum of measurement constructs is possible. As illustrated in the figure below, these constructs range from process measures to intermediate outcomes (such as physiologic measures), to intervention-specific outcomes, to population outcomes.
Types of Measures
Outcomes management, described by Ellwood as a “technology of patient experience,” was heavily promoted during the 1990s, but fell into disfavor because of the burden of routinely administering functional outcomes questionnaires to patients and capturing relevant clinical datasets from providers, particularly without widespread adoption of information systems designed to facilitate those processes. Both process and outcome measures offer important advantages (see figure above), and many advocate for the use of a variety of measures across this spectrum, with the addition of measures of consumer satisfaction and cost. When measurement is used optimally, it facilitates not only knowledge of the outcome, but also the reasons why a given outcome is achieved.